With research and education continuing to push the boundaries of the possible, yesterday’s standards for excellent health care are no longer good enough. The Duke Quality System is already working to remove obstacles to better quality, and breakthroughs in research and technology will set the bar even higher. Together, we will design and deliver remarkable, high value, personalized, and precise care, powered by advanced data sciences, clinical innovation, and a culture of kindness.
How we define success:
- Designing & delivering highest quality, personalized care as measured by clinical and patient-reported outcomes
- Patient experience and on-demand 24/7 access
- Value as defined by our constituents
Watch a Video About Leading in Clinical Excellence
Stories About Leading in Clinical Excellence
Duke/UNC Awarded Grant to Establish Joint Alzheimer’s Disease Research Center
Duke University and the University of North Carolina at Chapel Hill have been awarded funds from the National Institutes of Health to establish a prestigious Alzheimer’s Disease Research Center (ADRC), part of a federally-funded national network of similar centers.
The research center, one of 33 nationwide, will focus on identifying age-related changes across the lifespan that impact the development, progression and experience of Alzheimer’s and related dementias. The center will also identify how factors that arise in early- and mid-life contribute to racial, ethnic and geographic disparities in dementia.
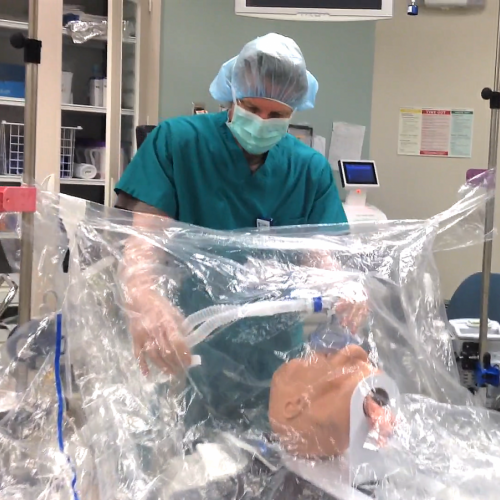
Alumnus Invents Disposable Intubation Drape
As a result of the COVID-19 pandemic, several products have entered the market aimed at protecting providers from respiratory droplets during airway manipulation. Tony Sandstrom, MSN’05, CRNA, noticed that, while these products generally work, they aren’t very adaptable to the provider. This observation led Sandstrom, who works at Duke University Hospital, to create the I-Drape, a disposable intubation drape.
“I always thought about things, coming up with improvements related to my profession as an anesthesia provider,” he said. “There are a few projects out there that people have thought of that look at how to protect the anesthesia provider from aerosolized particles or splatter up in the face when they are manipulating the airway, and none of them are user friendly, so to speak. I thought how about you have a completely different view of how to protect the provider.”
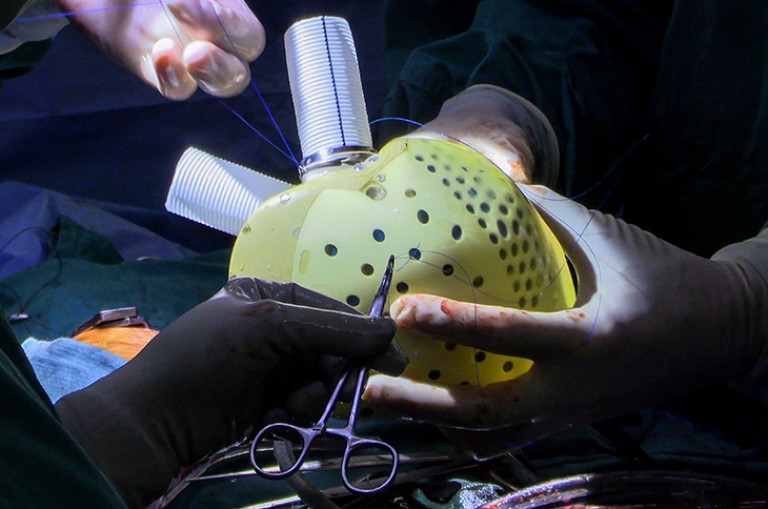
New Generation Artificial Heart Implanted in Patient at Duke – First in U.S.
A surgical team at Duke University Hospital, led by Drs. Jacob Schroder and Carmelo Milano, successfully implanted a new-generation artificial heart in a 39-year-old man with heart failure, becoming the first center in North America to perform the procedure.
This artificial heart has been studied in Europe, where it is approved for use. Last year, the company received FDA approval to begin studies in the U.S. to potentially enroll 10 patients with end-stage biventricular heart failure.
Assessment tool aids nurses with diagnosing delirium
An enhanced assessment tool is making it easier for nurses in intensive care units (ICUs) at all three Duke University Health System hospitals to identify patients experiencing delirium. Delirium impacts a patient's state of mind, causing confusion and disorientation. Patients may also be less responsive and less communicative.
“It's really important to identify patients with delirium because it increases their risk for falls, long-term impairment and mortality," said Myra Ellis, MSN, RN, CCRN-CSC, a clinical nurse IV in Duke University Hospital's cardiac ICU.
Team launches app to help prevent sepsis in patients
The Duke Institute for Health Innovation helped empower Duke University Hospital nurses to improve quality of care and make monitoring at-risk sepsis patients easier than ever.
"Sepsis Watch," is led by a team of nurses who collaborated with a group of providers to create and roll out an app and teach peers. It analyzes patient history and uses 32 million data points to identify patients at risk for developing sepsis, a life-threatening reaction to an infection, with more than 90 percent accuracy.
Capacity, Access and Real-time Engagement: CARE hub
This innovative tool allows users to access Tiles that display real-time data about our inpatients and available resources. We are proud of the CARE hub team for supporting our health system with the Capacity, Access and Real-time Engagement we need to ensure that the right patients are receiving the right care at the right time.
This one-minute video explains more about our CARE hub and how this program is enhancing patients’ access to our services and improving their experience.
Robot Helps Provide Human Connection During COVID-19
A Duke Raleigh Hospital case manager used a telepresence robot called JaMMeR to collaborate with her colleagues and see her Intensive Care Unit (ICU) patients while she works remotely during the COVID-19 response.
JaMMeR has been used for the last few years in an educational setting at the Duke University School of Nursing. This is the first time JaMMeR is being feasibility tested by the Duke University School of Nursing in a clinical setting, piloted at Duke Raleigh Hospital, to see how it might help augment face-to-face patient care.
Duke to Lead National Center for Virtual Imaging Trials
A new center in Duke’s School of Medicine provides scientists and physicians with the tools to use digital models of patients to assess the effects of imaging technologies and applications.
Launched this spring, the Center for Virtual Imaging Trials (CVIT) is supported by a five-year grant from the National Institutes of Health (NIH) and is directed by Ehsan Samei, PhD, professor in the departments of Radiology, Physics, Biomedical Engineering, and Electrical and Computer Engineering.
Study Shows Smartphone App Can Identify Autism Symptoms in Toddlers
A digital app successfully detected one of the telltale characteristics of autism in young children, suggesting the technology could one day become an inexpensive and scalable early screening tool, researchers at Duke University report.
The research team created the app to assess the eye gaze patterns of children while they watched short, strategically designed movies on an iPhone or iPad, then applied computer vision and machine learning to determine whether the child was looking more often at the human in the video, or objects.







.png)